INTRODUCTION TO NPWT
The management of difficult to heal wounds has always been a cause of concern for the treating clinicians. There has been a tremendous increase in the number of patients presenting with difficult to heal wounds. The conventional techniques have been in use since a long time for the management of these wounds, yet desired results are not achieved always. Thus a newer novel technique which might be useful in the difficult to heal wounds and delivering at par or better results as compared to the conventional techniques is the need of the hour. Despite numerous advances, chronic and other difficult to manage wounds continue to be a challenge for the clinicians. The relatively newer technique negative pressure wound therapy (NPWT) is very promising and also useful in the management of difficult to heal wounds.
The use of controlled levels of negative pressure application has been shown to accelerate debridement and promote healing in various types of wounds. This optimum level of negative pressure appears to be around -125 mmHg below ambient and there is evidence that this is most effective if applied in a cyclical fashion. Earlier studies used more conventional methods such as a wall suction apparatus or surgical vacuum bottles for creating the negative pressure. However, there were multiple problems present in the use of these conventional methods such as non-regulated pressure, high protein loss, cross contamination from infected patients, also the mobility of the patient was restricted.
Hence we introduced the commercial system for promoting negative pressure wound therapy also known as vacuum therapy, vacuum sealing or topical negative pressure therapy. This equipment called CCNPWT Wound Management system was designed to overcome the problems associated with conventional methods for the creation of negative pressure. The heart of the system is a microprocessor-controlled vacuum unit that is capable of providing controlled levels of continuous or intermittent sub-atmospheric pressure ranging from
-20mmHg to -220 mmHg.
NPWT is an efficacious & cost-effective management approach for almost all wound etiology such as pressure ulcers, trauma wounds, acute & chronic wounds, diabetic foot ulcers, venous leg ulcers, burns, post-surgical wounds, pre & post-op flaps/grafts.
MECHANISM OF ACTION
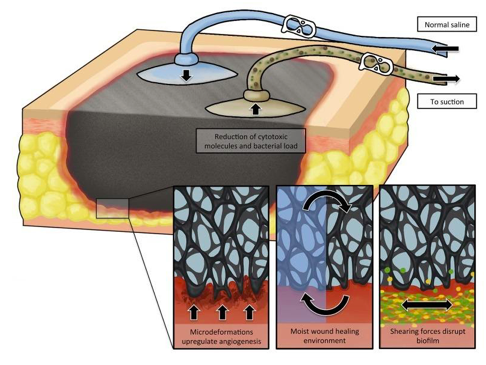
The principle of NPWT involves extending the usually narrowly defined suction effect of drainage across the entire area of the wound cavity or surface using an open-pore filler that has been fitted to the contours of the wound. To prevent air from being sucked in from the external environment, the wound and the filler that rests inside or upon the wound are hermetically sealed with an airtight adhesive polyurethane drape that is permeable to water vapour, transparent, and bacteria proof. A connection pad is then applied over a small hole that has been made in the drape and connected to a vacuum source by means of a tube (Fig 1).
Fig 1. Mechanism of action of Negative pressure Wound Therapy
Two main theories prevail regarding the mechanism of action of NPWT used in conjunction with reticulated open cell foam:
- The first is based on the theory that tissue strain caused by NPWT has a stimulatory effect on cellular proliferation.
- This theory is supported by the fact that tissues have been shown to undergo a 5-20% strain when subjected to NPWT.
- This level of strain is assumed to proactively cause cell division and angiogenesis.
- The second theory is focused on the effects of NPWT on the mechanical removal of extracellular fluid and oedema.
- By actively removing fluid at the wound bed it is felt that the local micro-circulation is improved and secondary necrosis is reduced.
This hypothesis is supported by studies which have shown reduced need for debridement at the time of ‘second look’ for wounds treated with NPWT. It is also supported by in vivo studies using a porcine model which have demonstrated acceleration in capillary formation and increase in luminal area in wounds treated with NPWT
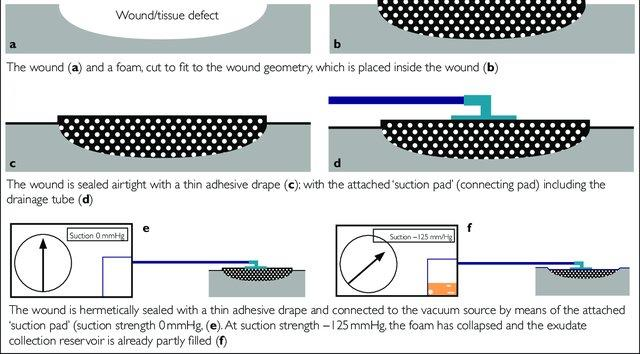
Fig 2. Dressing application technique
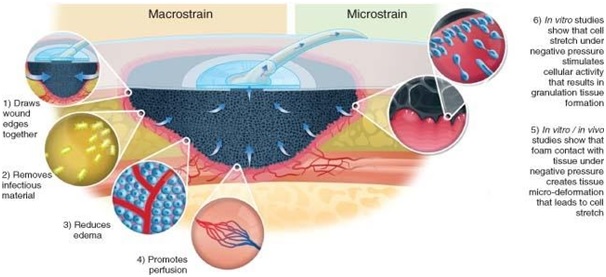
NPWT acts in different ways to promote wound healing. The wound is subject to suction pressure that is propagated through the wound filler to the wound bed. This suction drains exudate from the wound and creates a mechanical force in the wound edges that result in an altered tissue perfusion, angiogenesis and the formation of granulation tissue. Some of the mechanisms of action have been demonstrated experimentally and clinically.
The effects of NPWT on open wound can be summarised as follows:
- Reduction of the wound area due to negative pressure acting on the foam, pulls together the edges of the wound (wound retraction)
- Stimulation of granulation tissue formation in an optimally moist wound environment; in several situations even over brady trophic tissue such as tendons and bone NPWT was able to stimulate granulation tissue formation
- Continuation of effective mechanical wound cleansing (removal of small tissue debris by suction)
- Effective biochemical reduction of the fluid concentration of wound healing-impairing proteases (such as elastase)—in the first days
- Reliable, continuous removal of wound exudate (and, consequently, fewer dressing changes) within a closed system
- Pressure-related reduction of interstitial oedema with consecutive improvement of microcirculation, stimulation of blood flow and oxygenation
- Hygienic wound closure—bacteria proof wound dressing for sealing the wound so no external bacteria can enter the wound and the patient’s own wound bacteria are not spread.
- This is particularly important in the event of contamination with problematic bacteria, as in patients with meticillin-resistant Staphylococcus aureus (MRSA)-infected wounds. Thus, it
- also reduces the risk of cross-infections and development of resistance within the hospital
- Transparent dressing permits continuous clinical monitoring of the surrounding skin through the film with which the wound has been sealed
- Odourless and hygienic dressing technique; constant seeping through the dressing onto the patient’s clothing and bedding can be avoided, reducing demands on the nursing staff
- Reduction in the number of required dressing changes (only necessary every two to three days), which reduces nursing time requirements, particularly in patients with exudating wounds.
Patient comfort
• Easy and early patient mobilisation
• Visually appealing dressing method due to clean, exudate-free dressing conditions even during mobilisation.